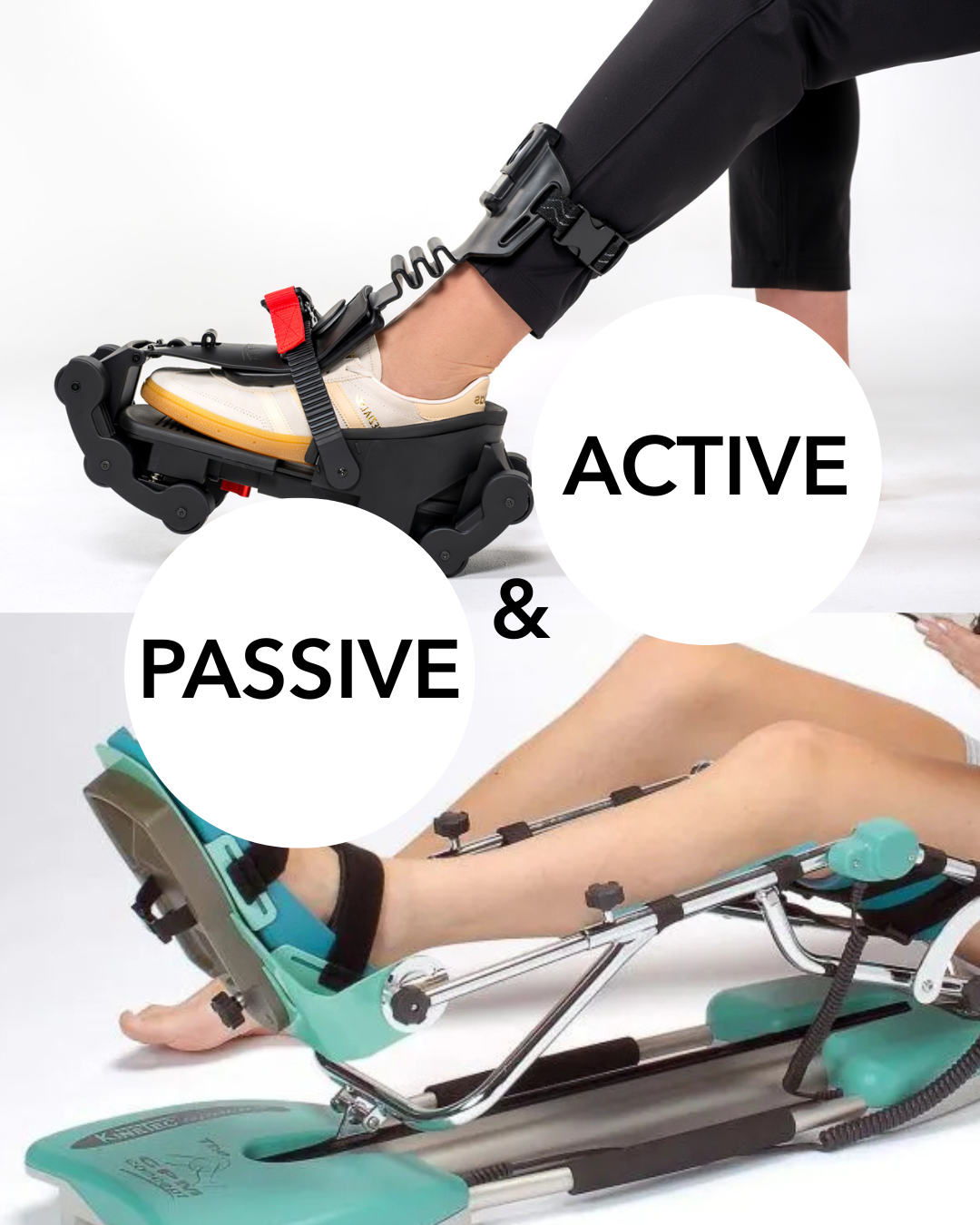

When recovering from surgery or injury, movement is medicine. But not all movement is the same. In rehabilitation, two key approaches are passive and active movements – each playing a critical role at different stages of recovery.
Using examples like the CPM and the MAXM Skate, let’s explore how these approaches differ, when to use them, and how combining both can optimise recovery outcomes.
Passive movement occurs when a joint is moved without the patient actively engaging their muscles.
The movement is generated by an external force – usually a therapist or rehabilitation device.
A great example of passive movement technology is the CPM (Continuous Passive Motion) machine. CPM devices are commonly prescribed after procedures such as :



Active movement requires the patient to engage their own muscles to create motion. This type of rehabilitation promotes strength, neuromuscular control, coordination, and long-term functional recovery.
The MAXM Skate is designed to support controlled active rehabilitation. It allows patients to perform guided sliding exercises that :

The combination of passive and active movement is recommended in rehabilitation because it addresses both tissue healing and functional recovery at the same time.
Passive movement – such as with a Knee CPM – helps maintain joint range of motion, improve circulation, reduce stiffness, and protect healing structures in the early stages after surgery or injury.
However, passive motion alone does not restore strength or retain the nervous system.
Active movement, on the other hand, rebuilds muscle strength, improves proprioception, and re-establishes motor control, but can be difficult or painful too early in recovery.
When both are combined, patients receive guided, safe joint motion while also activating their muscles. This reduces fear, promotes better movement quality, and accelerates functional progress.
Clinically, the combination bridges the gap between protection and performance, making recovery more efficient, more complete, and more sustainable.


MedFac UK Ltd
7 Redan Hill Industrial Estate, Redan Road,
Redan Road,
Aldershot,
GU12 4SJ
Tel: +44 (0) 3330 347400
Company Registration: 08608060
VAT Number: GB169722769
Subscribe today for our latest updates
Register for all our latest product news, information and services
Accepted Payment methods:
![]()
Copyright ©2026 - Kinetec Medical Products Ltd